Best Phakic IOL Surgery In D.N Nagar, Andheri, Mumbai
A phakic intraocular lens (PIOL) is a special kind of intraocular lens that is implanted surgically into the eye to correct myopia (nearsightedness). It is called “phakic” (meaning “having a lens”) because the eye’s natural lens is left untouched. Intraocular lenses that are implanted into eyes after the eye’s natural lens has been removed during cataract surgery are known as pseudophakic. Phakic intraocular lenses are indicated for patients with high refractive errors when the usual laser options for surgical correction (LASIK and PRK) are contraindicated. Phakic IOLs are designed to correct high myopia ranging from −5 to −20 D if the patient has enough anterior chamber depth (ACD) of at least 3 mm.
Three types of phakic IOLs are available:
Angle-supported
Iris-fixated
Sulcus-supported intraocular lens
An installed PIOL, without flash photography
LASIK can correct myopia up to -12 to -14 D. The higher the intended correction the thinner and flatter the cornea will be post-operatively. For LASIK surgery, one has to preserve a safe residual stromal bed of at least 250 µm, preferably 300 µm. Beyond these limits there is an increased risk of developing corneal ectasia (i.e. corneal forward bulging) due to thin residual stromal bed which results in loss of visual quality. Due to the risk of higher order aberrations there is a current trend toward reducing the upper limits of LASIK and PRK to around -8 to -10 D. Phakic intraocular lenses are safer than excimer laser surgery for those with significant myopia.
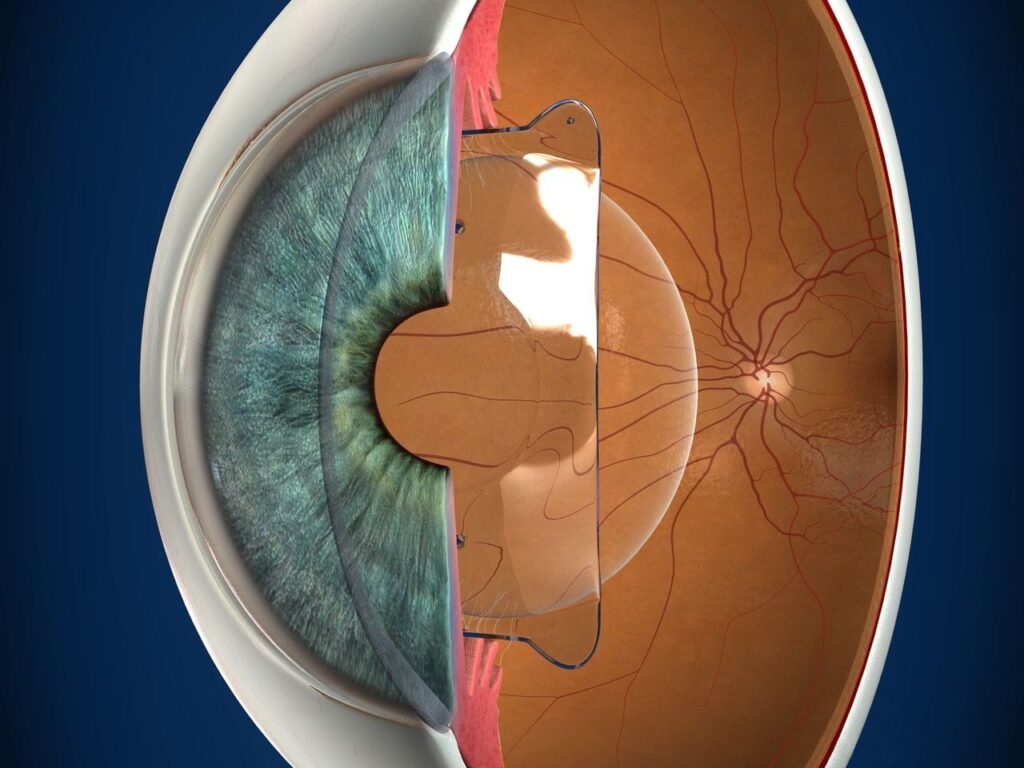
Advantages:
PIOLs have the advantage of treating a much larger range of myopic and hyperopic refractive errors than can be safely and effectively treated with corneal refractive surgery. The skills required for insertion are, with a few exceptions, similar to those used in cataract surgery. The equipment is significantly less expensive than an excimer laser and is similar to that used for cataract surgery. In addition, the PIOL is removable; therefore, the refractive effect should theoretically be reversible. However, any intervening damage caused by the PIOL would most likely be permanent. When compared with clear lens extraction, or refractive lens exchange the PIOL has the advantage of preserving natural accommodation and may have a lower risk of postoperative retinal detachment because of the preservation of the crystalline lens and minimal vitreous destabilization.
Disadvantages:
PIOL insertion is an intraocular procedure. With all surgeries there are associated risks. In addition, each PIOL style has its own set of associated risks. In the case of PIOLs made of polymethylmethacrylate (PMMA), surgical insertion requires a larger incision, which may result in postoperative astigmatism. By comparison, PIOLS made of collamer (a foldable gel-like substance) requires a very small incision due to the flexibility of the material and thus significantly reduces astigmatism risk. In the cases where refractive outcomes are not optimal, LASIK can be used for fine-tuning. If a patient eventually develops a visually significant cataract, the PIOL will have to be explanted at the time of cataract surgery, possibly through a larger-than-usual incision.
Another concern is progressive shallowing of the anterior chamber which normally occurs with advancing age due to the growth of the eye’s natural lens. Multiple studies have shown a 12-17 µm/year decrease in the anterior chamber depth with aging. If a phakic IOL patient is assumed to have a 50-year lifespan, the overall decline in ACD may add up to 0.6-0.85 mm, long-term data about this effect are not available. This concern is more important in ICL because it is implanted in the narrowest part of the anterior segment
Complications:
Glare and halos which may cause night time symptoms especially in patients with larger pupil diameters. Cataract which is the most crucial concern for the Sulcus-Supported PIOLs. According to FDA approximately 6% to 7% of eyes develop anterior subcapsular opacities at 7+ years following Implantable Collamer Lens implantation and 1% to 2% progress to clinically significant cataract during the same period, especially very high myopes and older patients. Endothelial cell loss especially for the anterior chamber PIOLs. A study observed a continual steady loss of endothelial cells of -1.8% per year. Pigment dispersion may be seen in iris-fixated and sulcus-supported PIOLs due to iris abrasion during pupillary movement. Other complications include glaucoma and PIOL dislocation or decentration.
Best LASIK Surgery In D.N Nagar, Andheri, Mumbai
LASIK eye surgery is the best known and most commonly performed laser refractive surgery to correct vision problems. Laser-assisted in situ keratomileusis (LASIK) can be an alternative to glasses or contact lenses. During lasik surgery, a special type of cutting laser is used to precisely change the shape of the dome-shaped clear tissue at the front of your eye (cornea) to improve vision. In eyes with normal vision, the cornea bends (refracts) light precisely onto the retina at the back of the eye. But with nearsightedness (myopia), farsightedness (hyperopia) or astigmatism, the light is bent incorrectly, resulting in blurred vision. Glasses or contact lenses can correct vision, but reshaping the cornea itself also will provide the necessary refraction.
Why it’s done?
LASIK surgery may be an option for the correction of one of these vision problems:
- Nearsightedness (myopia). When your eyeball is slightly longer than normal or when the cornea curves too sharply, light rays focus in front of the retina and blur distant vision. You can see objects that are close fairly clearly, but not those that are far away.
- Farsightedness (hyperopia). When you have a shorter than average eyeball or a cornea that is too flat, light focuses behind the retina instead of on it. This makes near vision, and sometimes distant vision, blurry.
- Astigmatism. When the cornea curves or flattens unevenly, the result is astigmatism, which disrupts focus of near and distant vision.
If you’re considering LASIK surgery, you probably already wear glasses or contact lenses. Your eye doctor will talk with you about whether LASIK surgery or another similar refractive procedure is an option that will work for you
Risks
Complications that result in a loss of vision are very rare. But certain side effects of LASIK eye surgery, particularly dry eyes and temporary visual problems such as glare, are fairly common. These usually clear up after a few weeks or months, and very few people consider them to be a long-term problem.
Risks of LASIK surgery include:
Dry Eyes
LASIK surgery causes a temporary decrease in tear production. For the first six months or so after your surgery, your eyes may feel unusually dry as they heal. Dry eyes can reduce the quality of your vision. Your eye doctor might recommend eyedrops for dry eyes. If you experience severe dry eyes, you could opt for another procedure to get special plugs put in your tear ducts to prevent your tears from draining away from the surface of your eyes.
Glare
halos and double vision. You may have difficulty seeing at night after surgery, which usually lasts a few days to a few weeks. You might notice increased light sensitivity, glare, halos around bright lights or double vision. Even when a good visual result is measured under standard testing conditions, your vision in dim light (such as at dusk or in fog) may be reduced to a greater degree after the surgery than before the surgery.
Undercorrections
If the laser removes too little tissue from your eye, you won’t get the clearer vision results you were hoping for. Undercorrections are more common for people who are nearsighted. You may need another LASIK procedure within a year to remove more tissue.
Overcorrections
It’s also possible that the laser will remove too much tissue from your eye. Overcorrections may be more difficult to fix than undercorrections.
Astigmatism
Astigmatism can be caused by uneven tissue removal. It may require additional surgery, glasses or contact lenses.
Flap problems
Folding back or removing the flap from the front of your eye during surgery can cause complications, including infection and excess tears. The outermost corneal tissue layer may grow abnormally underneath the flap during the healing process.
Regression
Regression is when your vision slowly changes back toward your original prescription. This is a less common complication.
Vision loss or changes
Rarely, surgical complications can result in loss of vision. Some people also may not see as sharply or clearly as previously.
Conditions that increase risks
Certain health conditions can increase the risks associated with LASIK surgery or make the outcome less predictable. Doctors may not recommend laser refractive surgery for you if you have certain conditions, including:
- Autoimmune disorders, such as rheumatoid arthritis
- A weakened immune system caused by immunosuppressive medications or HIV
- Persistent dry eyes
- Recent changes in vision due to medications, hormonal changes, pregnancy, breast-feeding or age
- Inflammation of the cornea, lid disorders, eye injuries or eye diseases, such as uveitis, herpes simplex affecting the eye area, glaucoma or cataracts